How healthcare providers shape your health at every stage
TL;DR:
- Healthcare providers focus on prevention, diagnosis, treatment, and health education to improve long-term well-being.
- A “medical home” coordinates care, monitors health metrics, and prevents small issues from becoming serious.
- Building a strong relationship with local primary care supports personalized, proactive health management for all ages.
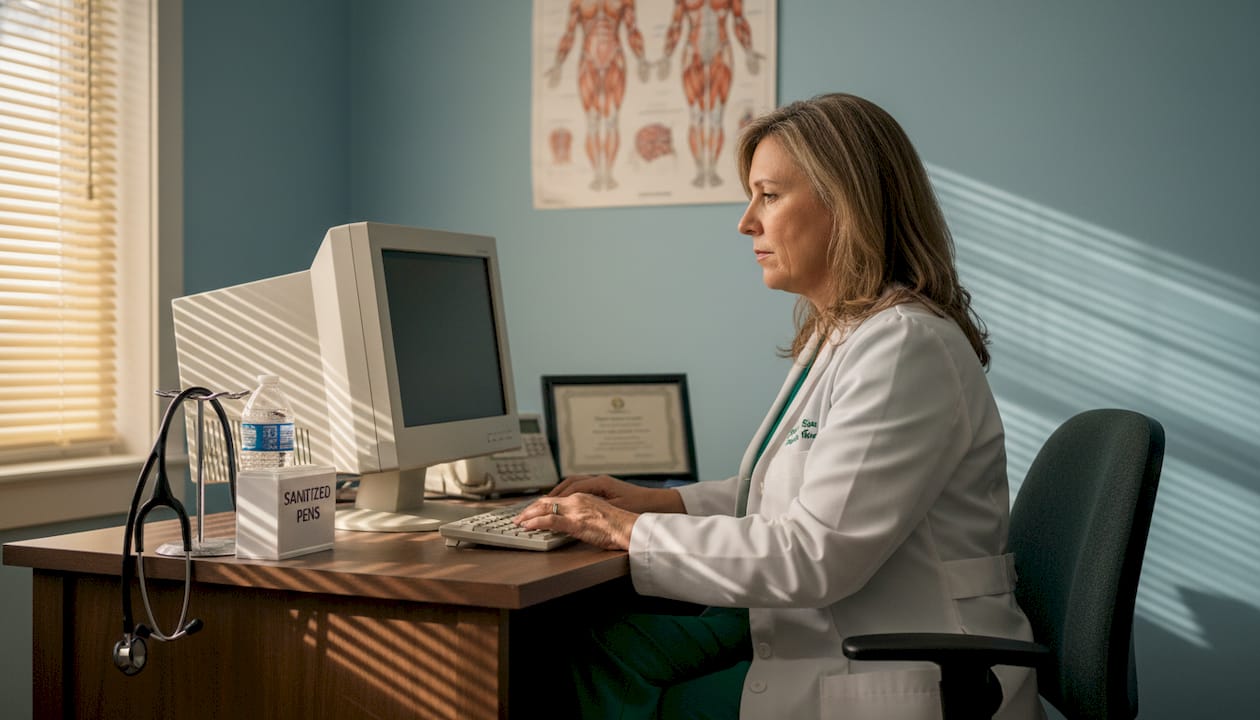
Most people only think about calling their doctor when something goes wrong. A cough that won’t quit, a nagging pain, or a worrying test result sends them through the door. But that picture misses the most important work your healthcare provider does every single day, which is quietly preventing those problems from becoming serious in the first place. For residents of North Bergen and Secaucus, understanding this broader role is the first step toward getting the most out of the care available to you right here in your community.
Table of Contents
- Understanding the role of healthcare providers: Beyond treating illness
- Primary care as your health navigator
- Tackling challenges: Diagnostic uncertainty and acute care in primary settings
- Personalized preventive and chronic care: Collaboration for better outcomes
- Why the healthcare provider’s role must evolve locally
- Connect with comprehensive care for your family
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Holistic health partners | Healthcare providers support your well-being far beyond treating illness by guiding prevention and ongoing care. |
| Primary care as coordinator | A trusted provider coordinates all aspects of your health, simplifying access to services and advice. |
| Innovation meets experience | Teams and technology like AI help address care challenges, but relationships and skilled judgment remain central. |
| Personalization is vital | Collaborative care plans tailored to individuals and families drive better long-term health outcomes. |
| Invest in prevention | Prioritizing primary and preventive care keeps communities like North Bergen and Secaucus healthier. |
Understanding the role of healthcare providers: Beyond treating illness
There is a persistent idea that healthcare providers exist mainly to fix problems. That thinking is understandable, but it leaves out the deeper, ongoing commitment that a good provider makes to your long-term well-being. In reality, your provider plays several distinct roles at once, and each one matters to your health in a different way.
Healthcare providers offer a combination of prevention, diagnosis, treatment, and health education, woven together into a continuing relationship with you and your family. Prevention might mean making sure you are up to date on vaccines, or catching high blood pressure before it causes a stroke. Diagnosis means working through symptoms systematically to find the right answer, not just the quickest one. Treatment goes far beyond writing a prescription, often including lifestyle guidance, referrals, and long-term monitoring. And education means helping you understand what your numbers mean, what your risks are, and what you can do about them.
As primary care explained, primary care acts as the first point of contact and the ongoing advocate for your health across all life stages. Whether you are a young adult managing your first health concerns, a parent tracking your child’s development, or an older adult balancing multiple conditions, your primary care provider stays involved at every step. The value of family care options like these is that they tailor support across different ages, backgrounds, and health situations, so no one in the household falls through the cracks.
“Primary care serves as a ‘medical home’ and is crucial for preventing complications,” according to healthcare quality leaders, who note that stronger investment here reduces strain across the entire health system. Source
Think of the conditions your provider monitors on a regular basis:
- Blood pressure and cholesterol levels
- Blood sugar trends for diabetes risk or management
- Weight and body mass, tied to heart disease and joint health
- Mental health screening and emotional well-being
- Cancer screenings appropriate for your age and family history
- Immunizations and travel health preparations
Each of these areas, addressed consistently and early, has a measurable effect on whether small problems grow into serious ones.
Primary care as your health navigator
Once you understand the full scope of a provider’s role, the concept of a “medical home” becomes clear. This is not a physical place so much as a philosophy of care, where one team knows your complete picture and takes responsibility for coordinating everything connected to your health.
Your medical home keeps central records of your conditions, medications, allergies, and past treatments. It schedules periodic reviews to check whether your health is trending in the right direction. When you need a specialist, your primary care team provides context and follows up afterward to make sure new recommendations fit your overall plan. This coordination prevents the kind of fragmented care where the cardiologist and the endocrinologist never talk to each other, and you end up managing the gap yourself.
As medical care processes in NJ demonstrate, routine screenings and check-ins are the backbone of this system. Catching an issue early, like a pre-diabetic blood sugar reading or a slightly elevated blood pressure, gives your provider time to act before the situation becomes urgent. Referrals happen faster and with more context when your provider already knows your history.
The table below shows the types of routine reviews that a primary care provider typically manages, and how often they are recommended for most adults:
| Health area | Recommended frequency | What it helps catch |
|---|---|---|
| Blood pressure check | Every visit or annually | Hypertension, cardiovascular risk |
| Blood glucose screening | Every 1 to 3 years | Prediabetes, type 2 diabetes |
| Cholesterol panel | Every 4 to 6 years (more often if at risk) | Heart disease risk |
| Colorectal cancer screen | Starting at age 45 | Early-stage colon cancer |
| Depression screening | Annually | Mood disorders, mental health needs |
| Bone density scan | Age 65+, or earlier if at risk | Osteoporosis, fracture risk |
For those already managing conditions like diabetes or hypertension, primary care takes on an even more active role. Your provider tracks how well your treatment plan is working, adjusts medications when needed, and connects you with education or support programs. Understanding how Medicare primary care coverage works, and how to use your insurance and access effectively, can make these ongoing relationships easier to maintain without financial stress.

As primary care funding experts note, primary care as a “medical home” prevents complications but needs better funding and reimbursement to remain sustainable over the long term. That context matters to you as a patient because it highlights just how valuable and sometimes fragile this system is.
Here are four practical steps every North Bergen and Secaucus resident can take to build a strong relationship with a primary care provider:
- Schedule an annual wellness visit, even when you feel completely well.
- Bring a written list of all medications, including supplements, to every appointment.
- Share family health history, since genetic risk factors affect screening recommendations.
- Follow up after referrals and make sure your primary care provider receives specialist notes.
Pro Tip: If you have not seen a provider in more than a year, start with a full wellness check rather than waiting for a problem to arise. That first visit sets a baseline that makes every future appointment more useful.
Tackling challenges: Diagnostic uncertainty and acute care in primary settings
Even with the best care systems in place, healthcare providers face real obstacles. Diagnosis is rarely as simple as running one test and getting a clear answer. Many conditions share symptoms. Patients describe the same sensation in completely different ways. And not every necessary tool is available in a primary care setting.
Diagnostic uncertainty is addressed using scales like PRUS and MDMQ, but there is a recognized lack of acute care assessment tools specifically designed for primary care settings. This means providers must make careful judgment calls, often under time pressure, using the information they have rather than the ideal set of resources.
The table below compares common approaches to managing uncertainty in primary care:
| Approach | Strengths | Limitations |
|---|---|---|
| Structured scales (e.g., PRUS, MDMQ) | Standardizes assessment, reduces guesswork | Not always designed for acute primary care situations |
| Team-based consultation | Brings in multiple perspectives, catches blind spots | Requires coordination and time |
| AI-assisted decision support | Flags patterns across large data sets quickly | Needs human oversight, not yet universally available |
| Watchful waiting with follow-up | Avoids unnecessary tests, preserves patient trust | Can delay care if symptoms change rapidly |
Team-based care is one of the most practical answers to this challenge. When nurses, physician assistants, and specialists collaborate in real time, the collective knowledge available to each patient goes up significantly. The rise of AI-assisted tools is also beginning to help providers flag unusual patterns and reduce the risk of a missed diagnosis, though these tools work best alongside, not in place of, clinical judgment and experience.
Understanding the distinction between situations that call for urgent vs. primary care helps you make better decisions when symptoms appear, and it helps your primary care team serve you more effectively by seeing you at the right time with the right information.
Current challenges affecting North Bergen and Secaucus residents include:
- Longer wait times when providers are stretched thin
- Limited availability of after-hours primary care for acute concerns
- Coordination gaps when multiple specialists are involved
- Patients unsure whether to go to urgent care or call their regular provider
Pro Tip: Ask your provider directly how they approach tricky or unclear symptoms. A good team will explain their reasoning process and what signs would lead them to investigate further.
Personalized preventive and chronic care: Collaboration for better outcomes
Understanding the obstacles providers face makes the commitment behind good care even more meaningful. When a provider builds a personalized plan for you, it reflects both clinical knowledge and genuine effort to work within real limitations.
Individualized care plans pull together screenings, patient education, and lifestyle support into a single, connected approach. Rather than treating your cholesterol in isolation or your weight as a separate issue, a strong care team sees how these factors interact and addresses them together. That integrated approach is what distinguishes good primary care from a series of disconnected appointments.
Collaboration makes this possible. Nurses provide day-to-day education and monitoring. Registered dietitians support patients managing diabetes or heart disease. Behavioral health professionals address stress, depression, and habits that affect physical outcomes. Investment in preventive care, rather than budget cuts to these support roles, directly shapes how effective care teams can be for people managing chronic conditions.
For those navigating long-term conditions, resources like a thorough chronic care guide and practical chronic care tips give you a clearer picture of what to expect and how to participate actively in your own care. Similarly, learning how practices are improving preventive care helps you understand what a well-run care team looks like, so you can recognize and appreciate it when you find one.
Here are four ways you can actively participate in your own personalized care plan:
- Tell your provider about your day-to-day routines, including sleep, diet, activity, and stress.
- Ask specifically what health goals they would prioritize for you in the next six months.
- Request written summaries of your care plan so you can review it at home.
- Check in between appointments if something changes, rather than waiting for the next scheduled visit.
Pro Tip: Set one specific, measurable health goal with your provider at each visit. Vague goals like “eat better” are harder to track than concrete ones like “reduce sodium to under 2,000 mg per day.” Specific targets make progress visible and keep motivation high.
Why the healthcare provider’s role must evolve locally
Here is an honest observation that goes beyond what most health articles will say: technology alone will not fix what our local healthcare system needs most. The conversation around AI, digital records, and telehealth is important, but it can crowd out a more fundamental need, which is steady funding, well-supported care teams, and real relationships between patients and providers.
AI and workforce shifts show that investment in people, not just technology, creates sustainable improvement in care. Provider burnout is real in communities like North Bergen and Secaucus, where providers often carry heavy caseloads while reimbursement rates for primary care lag behind specialty services. When good primary care providers burn out or leave the practice, patients lose continuity. That loss is harder to measure than a test result, but its impact on long-term health outcomes is significant.
What the future of local healthcare genuinely needs is a combination of things: patient-centered medical homes that are properly resourced, community-wide preventive programs that reach people before they develop complications, and a care culture that values the ongoing relationship between a patient and their provider as much as it values any single procedure or technology.
For residents of North Bergen and Secaucus, the most powerful thing you can do is engage consistently with the healthcare available locally, build a relationship with a primary care team you trust, and advocate for the kind of care that goes beyond quick fixes. That approach, repeated across a community, is what moves the needle on population health.
Connect with comprehensive care for your family
Taking what you now know about the provider’s role, the natural next step is finding a care team that actually delivers on all of it.
Garden State Medical Group serves North Bergen and Secaucus with a coordinated, multidisciplinary approach designed for exactly the kind of care described throughout this guide. From routine checkups and preventive screenings to specialist referrals and long-term chronic care management, the team here brings everything under one roof. You can explore primary care services tailored to individuals and families, or browse personalized health programs covering diabetes management, bone health, lung health, and weight management. Scheduling a visit is straightforward, and the team is ready to help you take a more proactive role in your health starting today.
Frequently asked questions
What is the difference between preventive and primary care?
Primary care manages ongoing health, coordinates treatment across conditions, and acts as your central medical resource, while preventive care focuses specifically on screenings, vaccinations, and early interventions to stop illness before it starts.
How can I find a primary care provider in North Bergen or Secaucus?
Check with local medical groups like Garden State Medical Group or contact your insurance provider for a list of in-network primary care clinics in the area that are currently accepting new patients.
Why is there a focus on teamwork and technology in healthcare today?
Modern care is too complex for any single provider to manage alone. AI-assisted tools and optimized teams allow providers to handle routine care efficiently while focusing their judgment on the complex decisions that truly need clinical experience.
What should I ask my provider about chronic care?
Ask how your care team tracks your progress over time, what specific goals they recommend for your condition, and what changes in your daily routine would have the biggest impact on your long-term health.
Is investment in primary care really worthwhile for my family?
Absolutely. Strong primary care investment prevents complications and supports better health across all age groups, reducing both the personal burden of illness and the overall cost of care over time.
