NJ Medicaid Eligibility: Who Qualifies and How in 2026

TL;DR:
- Medicaid eligibility in New Jersey varies based on age, disability status, household size, and income, with distinct pathways such as MAGI and non-MAGI. These standards update annually, and understanding which group you belong to is essential for accurate qualification. Applying year-round, staying current with policy changes, and ensuring proper documentation can improve access to necessary healthcare services.
Medicaid eligibility in New Jersey is not as straightforward as most people assume. Your neighbor with a similar household size and income might qualify under entirely different rules than you do, simply because of age, disability status, or the specific program they are applying for. Eligibility depends on income and household size and can shift from year to year based on state and federal updates. This guide walks you through New Jersey’s current Medicaid rules, who qualifies, how the financial tests work, and what steps to take if you think you or a family member may be eligible in 2026.
Table of Contents
- How Medicaid eligibility works in New Jersey
- Understanding MAGI and non-MAGI eligibility pathways
- Current income limits and household rules for NJ Medicaid (2026)
- Special eligibility routes: long-term care and medical need
- How and when to apply for Medicaid in New Jersey
- A realistic perspective: Why Medicaid eligibility isn’t always simple in New Jersey
- Connecting Medicaid coverage with better healthcare in New Jersey
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Eligibility isn’t one-size-fits-all | New Jersey assesses Medicaid eligibility by income, household, and individual status, not just financial need. |
| MAGI vs. non-MAGI rules | Most residents qualify via income tax concepts, but seniors and disabled use different financial rules. |
| Standards update yearly | Income limits and program rules change each year, so check current standards before applying. |
| Medical needs matter too | Some programs factor in medical or functional needs on top of financial eligibility. |
| Year-round enrollment | You can apply for NJ Medicaid at any time, regardless of the calendar. |
How Medicaid eligibility works in New Jersey
New Jersey’s Medicaid program, officially called NJ FamilyCare, covers a wide range of residents. But the program does not use a single, uniform set of rules for everyone. Instead, eligibility is group-based and determined using different financial methodologies depending on your age, family status, and health condition.
Think of it this way: a 32-year-old parent, a 67-year-old retiree, and a 45-year-old with a serious disability might all need Medicaid, but each one will be evaluated using a different set of rules. The factors that matter most include your age, whether you have a disability, your family composition, and your household income.
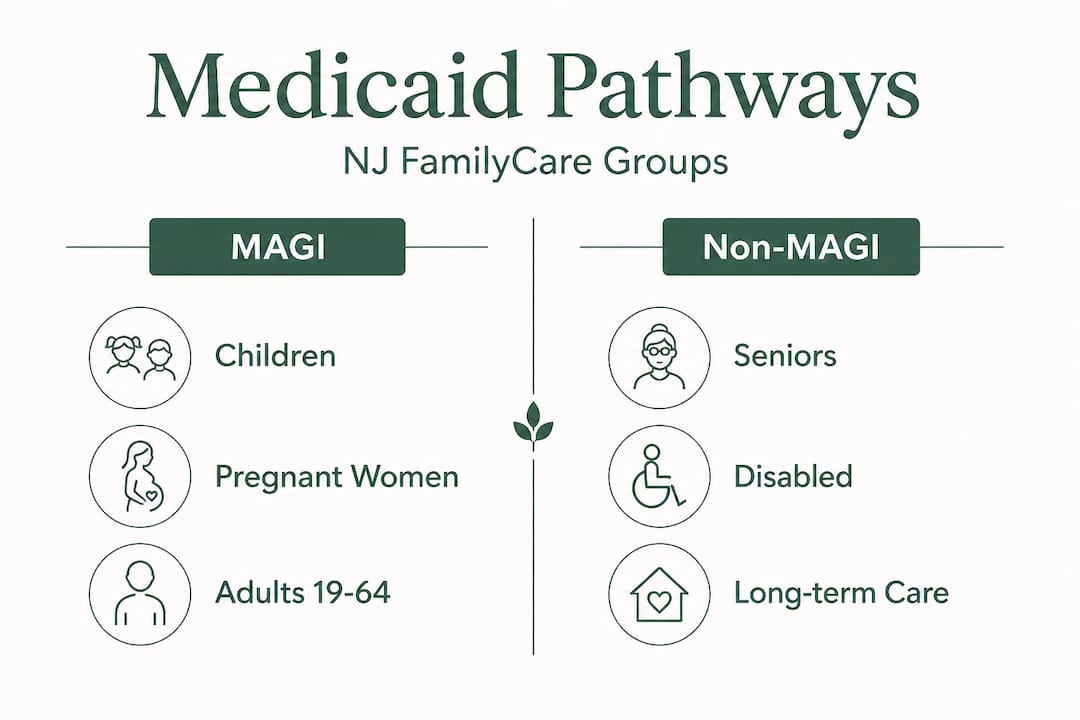
Most working-age adults, children, and pregnant women are assessed using what is called MAGI, which stands for Modified Adjusted Gross Income. This method aligns closely with how the IRS calculates income for tax purposes. For other groups, particularly seniors and people with physical or developmental disabilities, the state uses a separate set of criteria called non-MAGI rules, which may also take personal assets into account.
It is also important to understand that eligibility standards update annually, which means income thresholds that applied in 2025 may differ from the 2026 levels now in effect. Staying current with these updates can make the difference between qualifying and being turned away. You can find broader context about Medicaid healthcare access and chronic care in New Jersey if you want to understand how coverage connects to managing ongoing health conditions.
For most families, the key eligibility questions are: What group do I belong to? What financial method applies to my group? And does my income fall within the current limits? Once you answer those three questions, the path forward becomes much clearer. You may also want to review these NJ health insurance coverage tips for additional guidance on making the most of your options.
| Eligibility factor | Details |
|---|---|
| Age | Children, adults, seniors have separate rules |
| Disability status | Determines MAGI vs. non-MAGI pathway |
| Household size | Affects income limits directly |
| Income level | Compared against current FPL thresholds |
| Immigration/residency status | U.S. citizenship or qualified status required |
Understanding MAGI and non-MAGI eligibility pathways
With that background, it is essential to understand there is more than one way to qualify for Medicaid in New Jersey, depending on your circumstances. The two primary pathways are MAGI-based eligibility and non-MAGI-based eligibility, and knowing which one applies to you shapes everything from what documents you need to how long the process takes.
MAGI rules govern most ACA-related Medicaid eligibility, while older adults and people with disabilities use non-MAGI rules. MAGI is the more straightforward of the two for most working-age New Jerseyans. It counts your household’s taxable income the way your federal tax return would, excluding certain non-cash benefits. It does not consider your savings, property, or other assets. This means a young family with modest savings but a low income could still qualify without worrying about what they have in the bank.
Non-MAGI rules are different. Older adults and people with disabilities may be evaluated under non-MAGI rules, which look at both income and countable assets, sometimes called resources. This pathway is more detailed and can require additional documentation. It also tends to have lower income thresholds in some cases, though the trade-off is access to more specialized services like long-term care and nursing facility coverage.
Pro Tip: If you are helping an elderly parent apply for Medicaid and you are not sure which pathway applies, start by asking your local county Board of Social Services. They can tell you right away whether your family member will be evaluated under MAGI or non-MAGI rules, saving you significant time.
The groups that typically use MAGI include children under 19, pregnant women, and adults between 19 and 64 who are not eligible for Medicare and do not have a qualifying disability. The groups that generally fall under non-MAGI include adults 65 and older, individuals who receive Supplemental Security Income (SSI), and people who qualify for nursing facility or community-based long-term care. You can learn more about how Medicare and Medicaid options work together for older New Jerseyans, which is especially relevant for residents approaching or already in their senior years.
It is also worth knowing that some individuals may be eligible under either pathway, and New Jersey will typically evaluate you under the most favorable set of rules. Families with multiple members of different ages may find that children qualify through MAGI while a grandparent in the same home qualifies through the non-MAGI route. Understanding family health programs in NJ can help you see how these different pathways come together for multi-generational households.
| Feature | MAGI pathway | Non-MAGI pathway |
|---|---|---|
| Who it covers | Children, pregnant women, working-age adults | Seniors, disabled individuals |
| Income counting method | Adjusted gross income (tax-based) | Gross income plus asset review |
| Assets considered? | No | Yes |
| Connected to ACA expansion? | Yes | No |
| Application complexity | Moderate | Higher |
Current income limits and household rules for NJ Medicaid (2026)
The next logical question for New Jerseyans is: do your household and income line up with this year’s rules? The 2026 income limits are now in effect, and they are expressed as a percentage of the Federal Poverty Level (FPL). The FPL is a federal measure updated annually and used across many assistance programs to define low income.
NJ’s eligibility standards are updated annually, with 2026 levels now active. For most MAGI categories, New Jersey is generous compared to many other states. Children can qualify at income levels up to 355% of the FPL in some cases, while adults may qualify at lower thresholds depending on their category. The following table offers a simplified look at approximate income limits for common household sizes.
| Household size | Approximate monthly income limit (adults) | Approximate monthly income limit (children) |
|---|---|---|
| 1 | $1,732 | $4,122 |
| 2 | $2,340 | $5,570 |
| 3 | $2,948 | $7,016 |
| 4 | $3,556 | $8,462 |
These figures are approximate and may vary by specific program category. Always verify current limits directly with the state or a qualified benefits counselor.
When the state evaluates your household, who counts as part of it? Generally, your household includes yourself, your spouse if you are married, and any dependent children you claim on your federal tax return. It does not always include everyone living under the same roof. For example, a roommate or unrelated adult would not typically count in your household for Medicaid purposes, even if you share expenses.
New Jersey allows year-round enrollment in NJ FamilyCare, which is a significant advantage. Unlike private health insurance through the marketplace, you do not need to wait for an open enrollment period. If your income drops or your family situation changes at any point during the year, you can apply right away. This is especially important for residents who lose a job or experience other sudden changes. For more on checking Medicaid eligibility, including what to expect from the verification process, that resource can help you prepare.
Special eligibility routes: long-term care and medical need
Besides financial criteria, some New Jersey residents need to meet medical requirements to access long-term Medicaid programs. This section focuses on Long-Term Services and Supports, or LTSS, which covers things like nursing home care, assisted living programs, and home and community-based services.

For LTSS eligibility, income alone does not determine access. Applicants often need to meet a “nursing facility level of care” standard, which means a doctor or assessor confirms that the individual needs the kind of assistance typically provided in a nursing facility. This could involve limitations in daily activities like bathing, dressing, eating, or managing medications.
The specific activities evaluated are often called ADLs (Activities of Daily Living) and IADLs (Instrumental Activities of Daily Living). ADLs include basic self-care tasks, while IADLs cover things like managing finances, cooking, and using transportation. A formal assessment is typically required to document these limitations.
Income and resource limits for LTSS programs also differ from standard Medicaid. The asset thresholds are generally much lower, and certain asset transfers made within a “look-back period” (typically five years) may affect eligibility. This is why planning ahead is so important for older adults who anticipate needing long-term care services.
Pro Tip: If you or a loved one might need long-term care Medicaid in the next few years, speaking with a Medicaid planning attorney or benefits specialist now, before a crisis, can protect your eligibility and your family’s finances. Learn more about accessing NJ health programs to find resources closer to home.
How and when to apply for Medicaid in New Jersey
Once you know how you or your loved one might qualify, here is how to check eligibility and apply in New Jersey. The process is more manageable than many people expect, especially when you go in prepared.
-
Determine your eligibility group. Start by identifying which category you fall under: child, pregnant woman, working-age adult, senior, or person with a disability. This tells you which financial methodology applies.
-
Review the current income limits. Using the 2026 standards, compare your household’s monthly gross income against the limits for your category. Remember that household size affects the threshold significantly.
-
Gather your documents. You will typically need proof of income (pay stubs, tax returns), proof of identity (driver’s license or passport), proof of residency in New Jersey, and Social Security numbers for all household members.
-
Apply through the right channel. You can apply online through the NJ FamilyCare website, in person at your county Board of Social Services, or by mail. New Jersey residents can enroll year-round, so there is no need to wait for a specific window.
-
Stay informed about policy changes. Because eligibility policies can change due to federal and state updates, it is smart to check for updates at least annually, especially around the start of each calendar year. Renewing your coverage on time is equally important.
For a step-by-step walkthrough of what to expect in the process, the guide on NJ healthcare coverage steps can walk you through the insurance verification side of things as well.
Pro Tip: If you apply and are denied, you have the right to appeal. Many denials occur because of missing documentation rather than true ineligibility. Gather what was missing and reapply or request a fair hearing.
A realistic perspective: Why Medicaid eligibility isn’t always simple in New Jersey
Much of what is written about Medicaid eligibility focuses on the theory. But what does the process actually look like for real New Jersey residents navigating the system for the first time, or even the second or third time?
Here is something we see repeatedly: two families with nearly identical incomes and household sizes end up with different Medicaid outcomes. One qualifies, one does not. The reason is almost always a small but consequential detail, like whether one household includes a non-filing adult whose income is counted differently, or whether one applicant is enrolled in a qualifying disability program that opens a separate eligibility pathway.
The rules are detailed, and the details genuinely matter. This is not meant to be discouraging. It is meant to set realistic expectations so you go into the process with your eyes open rather than assuming the outcome is obvious.
Another reality: Medicaid eligibility rules and procedures can change due to federal and state policy shifts, sometimes mid-year and with relatively short notice for enrollees. The pandemic-era continuous enrollment protections that kept millions covered ended in 2023, and that unwinding process removed hundreds of thousands of people from Medicaid rolls nationally, many of whom were still eligible but lost coverage due to procedural issues. New Jersey navigated this more carefully than many states, but it demonstrated how external policy shifts can disrupt coverage even for people doing everything right.
The most proactive thing you can do is check your eligibility status annually, update your contact information with the state so you receive renewal notices, and review your income and household status whenever something major changes in your life. A job change, a marriage, a new baby, or a household member moving out can all affect your eligibility. For guidance on available medical care in NJ, knowing your coverage status upfront helps you make the most of every appointment and service.
Do not overlook the non-MAGI nuances, especially if someone in your family is aging or has a new disability diagnosis. Many families miss these pathways entirely because they assume the MAGI rules are universal. They are not, and that distinction can determine whether someone receives the long-term support they need.
Connecting Medicaid coverage with better healthcare in New Jersey
Understanding eligibility is only part of the equation. Using your Medicaid coverage effectively can dramatically improve your healthcare journey, especially for preventive care, chronic condition management, and specialist access.
At Garden State Medical Group, we welcome patients with a wide range of insurance coverage, including Medicaid. Whether you need primary care services for routine checkups, ongoing care for a chronic illness, or access to radiology and diagnostic testing, our North Bergen and Secaucus locations are equipped to serve you. We also offer specialized programs like our diabetes prevention and education program for patients managing blood sugar and metabolic health.
If you have recently qualified for Medicaid or are in the process of applying, we encourage you to schedule an appointment with one of our physicians. Getting connected to a consistent primary care provider is one of the most important steps you can take for your long-term health. Contact us through our website to learn more about services available to Medicaid patients in your area.
Frequently asked questions
What income counts toward Medicaid eligibility in New Jersey?
MAGI is used for most categories, including children, pregnant women, and working-age adults, while seniors and disabled residents are evaluated under non-MAGI rules that also consider assets.
Do Medicaid income limits change every year in New Jersey?
Yes, NJ updates Medicaid income levels annually, with 2026 standards now in effect as of January 1, 2026.
How is Medicaid eligibility different for elderly or disabled residents?
Non-MAGI pathways apply for elderly and disabled applicants, meaning the state reviews both income and countable assets, along with functional needs, rather than income alone.
Can I apply for NJ FamilyCare anytime during the year?
Yes, residents can enroll any time throughout the year. There is no open enrollment window for NJ FamilyCare, making it accessible even after a sudden change in circumstances.
What happens if Medicaid eligibility rules change while I’m enrolled?
When rules change over time, New Jersey typically notifies enrollees during renewal or redetermination periods. Keeping your contact information current with the state is the best way to stay informed and avoid gaps in coverage.
